I recently completed moderating my first LinkedIn Live discussion on a topic near and dear to my heart – Health Equity and Leading through Policy & Technology. The panel discussion was so rich and inspiring that I wanted to capture the highlights in a blog to share with everyone. Still, if you have the time to watch our 37-minute chat, you’re more than welcome to see the recording here.
The thinking and planning for this discussion began in November of 2021. It turns out that when you’re working with amazingly talented people, you must plan early. I was thrilled to be able to talk about health equity with:
- Ms. Valerie Mattison-Brown, Chief Strategy Officer for the Veterans Health Administration
- Dr. Umair Shah, Secretary of Health for the State of Washington Health Department
- Dr. John Balbus, Interim Director of the HHS Office of Climate Change and Health Equity
Defining Health Equity
Perhaps I should begin with defining health equity. Many turn to the CDC’s definition which states that “Health equity is achieved when every person has the opportunity to attain his or her full health potential.” The key word in this statement is opportunity which simply describes the set of circumstances that make something possible. Yet many people in our world cannot be described as having those enabling circumstances present in their lives. That deficiency can lead to unfair differences in access to health care, health promoting services, higher rates and increased severity of disease, shorter lifespans, and a lesser quality of life.
The Social and Structural Determinants of Health
Many refer to the contextual circumstances that either create or act as a barrier to opportunity as the social determinants of health. Others are advocating for the term structural determinants of health. I believe both are relevant. The social determinants of health are familiar to many and include the various conditions under which people are born, grow, live, work and age.
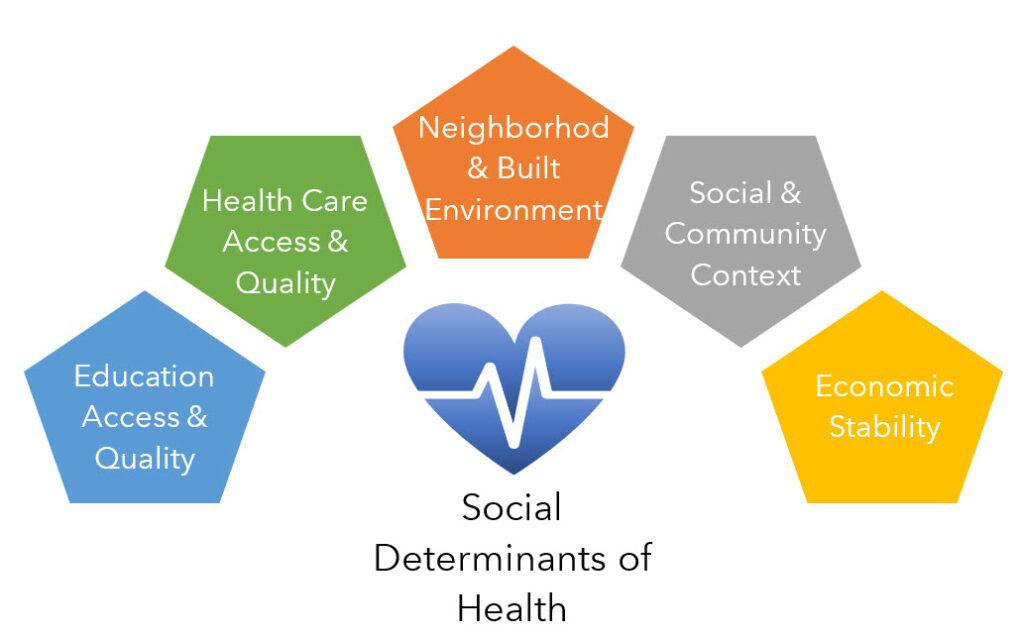
Using the term “structural determinants of health” provides a different, upstream lens into the causes of many social determinants of health. Structural determinants refer to the policies, programs, systems, and budget decisions that drive those downstream conditions we’re discussing. All these determinants vary spatially. That’s why I appreciate the vision statement from the Healthcare Information and Management Systems Society (HIMSS) which reads, “To realize the full health potential of every human, everywhere.” Implied in the HIMSS statement is that one must meet every human where they are in their health journey (fairness) and that place is important in the effort (context). We’ve all heard that your ZIP Code may be more important than your genetic code to your health outcomes. While it’s not a competition, the point is that the resources, access, and capacity to realize full health potential varies over place and time.
Why now?
During the panel, I asked Umair why things are so different now. After all, the social determinants of health are not new. Some form of social equity analysis and its relationship to health has been a part of the health field for more than 200 years. Umair eloquently made the point that while the pandemic did not start health inequities, it was very effective in shining a light on inequities throughout communities across the union. Not only was the light bright, but it demanded definitive action – a huge step beyond the former emphasis on research that enhances understanding of the nuances of inequity. Umair made it clear that GIS can support that action at every step – integrating data, presenting data with compelling maps, conducting surveillance activities, and implementing service delivery where it’s needed most.
Equitable Resource Allocation
If we drill down to just one part of this equation – service delivery – we can begin to understand some of the challenges associated with equitable resource allocation. Valerie spoke beautifully to the range of issues she considers when creating strategic plans to increase veteran access to health care. With over 9 million U.S. veterans and 96 healthcare markets, Valerie is doing her strategic planning for the largest integrated healthcare system in the country. This is no small job. To provide the most optimal access to healthcare, the Veterans Health Administration (VHA) considers the locations of their diverse veteran population across the country as well as ongoing migration patterns. I was surprised to learn that there has been a shift in the veteran population from the north to the southeastern and southwestern parts of the U.S. Providing care in the right places requires an ongoing study of movement and demographics.
Speaking of demographics, the veteran population continues to change regarding male/female population ratios, meaning that VHA must consider the health needs of women and how they are different from those of men. VHA is also keeping an eye on other potential vulnerabilities impacting their population such as food deserts where nutrition support may be needed. GIS is helping VHA connect the dots across the enterprise. Through location, they can bring all their information together to guide the direction of the organization.
Climate Change and Health Equity
While Valerie represented a focused ‘drill down’ approach, John Balbus gave us the opportunity to ‘drill up’ and see a bigger picture as he discussed the overlapping challenges of climate change and health equity. John’s comments really resonated when he spoke to the way that place integrates cumulative stressors and offers us a means to include and make sense of multiple factors across the spectrum of climate change and health equity. Looking at the figure below, combined with the social determinants of health noted above, one can begin to imagine multiple datasets that would be required to fully understand and act on health inequities associated with climate change.

Here’s an example. In the southwestern United States warmer temperatures have worsened drought conditions, leading to an arid and dusty landscape in many places. Combine these dry conditions with increasing dust storm activity in the area and you’ll see a significantly expanded spread of the Coccidioides spores that cause Valley fever. Those most at risk include agricultural and construction workers, firefighters, Black and Latino persons, persons with diabetes, elderly persons, incarcerated persons, migrant or undocumented farmworkers, and tribal communities. Furthermore, those with a serious case of Valley fever will also be at increased risk of developing severe COVID-19 disease and even co-infection with both. Valley fever and COVID-19 also have similar symptoms, making it hard to distinguish the two at the time of diagnosis. Yet, if a mistake is made, for example, mistaking Valley fever for COVID-19, the treatment course could worsen the underlying disease. You get the point, right? This is complicated.
John also noted that the solution space for climate change and health equity is hyper-local. So while we think and understand much of the overlap at the ‘drill up’ level, the local context matters for getting things done right for a particular community and its specific challenges. John argued that infrastructure investments, for example, need to be aligned and coordinated in a place-based manner. This is truly systems level thinking and I like it a lot!
The BRACE Framework
If you’re not already aware, John mentioned that the CDC has a framework called BRACE – Building Resilience Against Climate Effect. The BRACE Framework has the following 5 steps:
- Anticipate Climate Impacts and Assessing Vulnerabilities
- Project the Disease Burden
- Assess Public Health Interventions
- Develop and Implement a Climate and Health Adaptation Plan
- Evaluate Impact and Improve Quality of Activities
BRACE provides a logical methodology for broad systems thinking and GIS can support every step in the process. You might enjoy this story map that my colleague, Diana Lavery, worked on with me and experts from NOAA to understand heat impacts. You’ll see how it touches on the various steps from BRACE.
Not About Us, Without Us – Engaging Communities
All my panel experts, John, Valerie and Umair, spoke to the need to involve communities in solutions for improving their health. They spoke of empowering residents with tools that provide information and help them make their own decisions. They implored those of us in the field to bring in community members to shape policies and participate in the decisions that affect them. One of my new favorite sayings is “not about us, without us.” To me, that says it all.
Pondering our Future
There is a concern that’s been nagging me for some time now and our speakers articulated the issue and the options better than I ever have. I’m always wondering if the health sector, both in the United States and globally, will use what we’ve learned from the last two and a half years to leap-frog forward in our resilience and technologic savvy going forward. After all, we’ve exposed and clarified our gaps, created loads of solutions, and worked quickly to solve problems. Here’s what they said.
John acknowledged that we’re in a period of historic trauma – overlapping traumas – from COVID-19 to racial violence to extreme disasters from weather and war. Umair pointed out that we could react in a transactional way – something we’re good at, meaning that we ‘finish’ with the pandemic and move on to the next crisis, just getting things done, without benefit of reflection, debrief or the like. We might call this the pessimistic viewpoint. His more optimistic perspective is that we can choose to be transformational, taking the summation of everything we’ve learned – good and bad – and intentionally investing in transforming our health infrastructure and our society. Valerie aligns with the optimistic point of view as well, saying we NEED to be in the business of learning from what we’ve experienced. We don’t want to be left in 20th century thinking. And then speaking directly to what I needed to hear, John proposed that this time-period in our lives has been important enough that we WILL be inspired to act. If I can be of any service in this area, I’d like to be. My first offering is a book entitled, “Learning from COVID-19: Applying GIS for Pandemics.”
Learn More
Though our discussion lasted but 37 minutes, I found myself motivated to share the wisdom of my colleagues in this blog. You might also be interested in a new research brief that my Esri colleagues, Chris Thomas, Nicte Hernandez, and I worked on with the National Association of County and City Health Officials (NACCHO) called “Opportunities for Systemic Change: How Local Health Departments are Advancing Health Equity Through GIS.” There is much to learn and I welcome your comments and questions.

