
June 25, 2020 |
September 24, 2020

With a COVID-19 vaccine expected by fall 2020, governments around the globe must be ready to distribute vaccinations on a massive scale—an effort that includes the hurdles of meeting subzero storage requirements, prioritizing vulnerable communities, communicating with each other and the public, and ensuring equity across countries, counties, and cities.
Clearly, the work to safely develop and plan immunization in the US and around the world will require the most complex global vaccination campaign in history. At the pandemic’s onset and throughout 2020, government and healthcare leaders relied on Esri’s geographic information system (GIS) technology for real-time visualization dashboards, data sharing, analysis, and planning. The same GIS approach will prove crucial for vaccine distribution.
Right now, leaders can fine-tune vaccination scenario planning related to priority and delivery, assess logistics with public health and emergency management advisors, analyze supply chain capacity and operations, and determine a communication strategy. For all of these efforts, GIS will be foundational to help plan, implement, and manage efficient, equitable vaccine distribution.
In the US, for example, the Department of Health and Human Services (HHS), in coordination with Department of Defense (DoD) and the Centers for Disease Control and Prevention (CDC), recently provided a strategic vaccine distribution overview along with an interim playbook for state, tribal, territorial, and local public health programs and their partners.
The agencies outline next steps that include engaging with other leaders, stakeholders, and the public; distributing vaccines quickly and with transparency; ensuring safe administration and availability; and monitoring necessary data through an IT system capable of supporting and tracking distribution, administration, and other necessary data.
GIS is an integral part of that IT system, and will be central to vaccine distribution efforts, supporting engagement with stakeholders and the public as well as providing real-time awareness and transparency.
Here, we highlight five key ways GIS can support COVID-19 vaccine distribution to help health agencies and governments execute their plans and end this pandemic as quickly as possible.
Both of the leading vaccine candidates require cold storage, with one requiring ultra-cold storage at -70 degrees Celsius. Other factors such as parking, accessibility to vulnerable populations, distance from vaccine production facilities, traffic, and overall venue size will also impact which facilities can properly store and distribute a vaccine.
“States are currently surveying their systems to know where their sub-80 (Celsius) freezers are,” said Julie Swann, a professor of industrial and systems engineering at North Carolina State University, who was advising the CDC. “I would expect that kind of cold storage to be available at large hospitals, scientific research facilities, and some large pharmacies.”
The facilities Swann mentions are likely those already administering other vaccines in their normal course of business. These larger facilities may be prioritized in Phase 1 of the vaccine distribution process. During this phase, vaccines will be limited and focused first on people serving in healthcare settings who may have direct exposure to patients infected with COVID-19. Second will be those who work in essential jobs that keep society running (e.g. emergency and law enforcement personnel, food packaging and distribution workers, teachers and school staff, and childcare providers).
A larger vaccine supply is expected to be available to support Phase 2 of the distribution process. In that phase, additional facilities will be needed such as private provider offices, worksites, clinics, hospitals, health departments, retail settings, and senior centers. Mapping the breadth of potential facilities in the vaccination process is the first step to ensuring adequate population coverage.
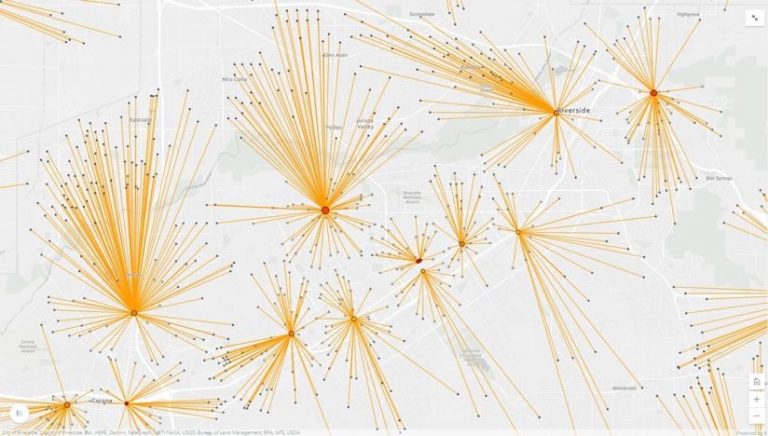
There won’t be enough doses of the vaccine immediately, so it’s important to be both strategic and ethical with the available resources. The proposed prioritization, as described above, ensures critical infrastructure workers—those most likely to be exposed to COVID-19—are first to be vaccinated.
The next group prioritized are those at increased risk for severe disease or death from COVID-19. This includes people in congregate living situations such as nursing homes and assisted living facilities, those who have underlying medical conditions or risk factors for severe disease like obesity, cancer and diabetes, and adults age 65 years and older.
The third group in the prioritization describes people who are at increased risk of contracting or transmitting the virus (listed in the CDC interim playbook as those experiencing homelessness or living in shelters, people working in educational settings or attending college/university, tribal communities and those from racial and ethnic minority groups, people living and working in congregate settings, and incarcerated individuals).
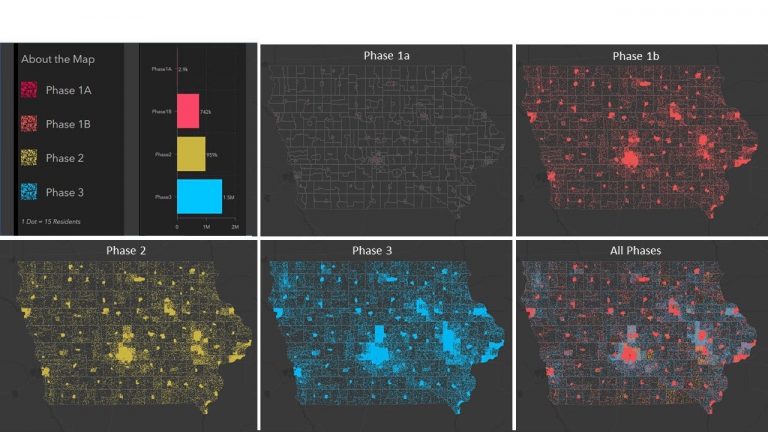
Health departments will need to develop a detailed view of the various priority populations across their jurisdictions. At the same time, they will need to assess any additional burdens the priority populations may face in receiving the vaccine, such as lack of transportation or barriers to communication for non-English speakers.
Beyond visualization, health departments will need actual population counts for total population and each priority group. To be most effective, those counts should be available in context. In other words, how many of the population are within 1 mile, a 15-minute walk, or a 30-minute drive of a vaccination venue. It will be critical to match facility capacity, vaccine supply, and population groups across locations to ensure all needs are met.
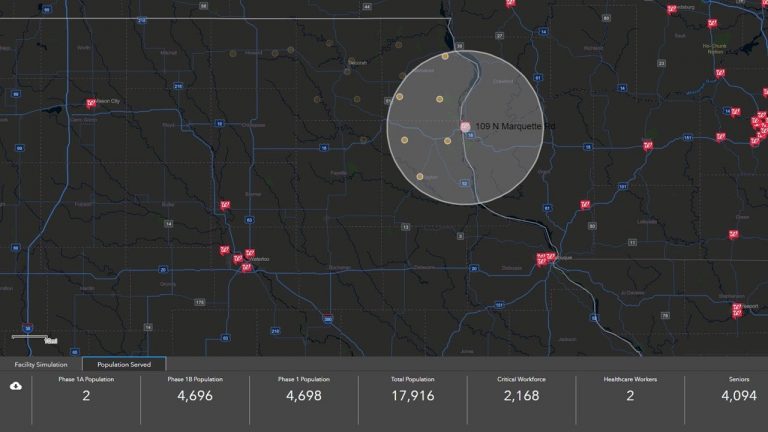
After communities have identified potential vaccine distribution facilities along with critical populations to prioritize, they will be able to see potential gaps and evaluate solution scenarios for mitigation.
It is possible and perhaps likely that in Phase 2 of the vaccine distribution plan, the general population’s desire to be vaccinated will overrun capacity in vaccination venues. Government leaders will have options to increase capacity by engaging new partners in the process and/or by siting Points of Dispensing (PODs) in strategic locations to meet demand. GIS technology has long been used for various types of site selection and is especially useful when considering complex criteria, such as accessibility, population makeup, ingress and egress, budget, and more.
There are special populations which should be targeted for more intentional outreach, such as those with limited access to vaccination venues in rural communities, people with disabilities, under- or uninsured people, people experiencing homelessness, and others who may be less likely to seek out vaccination when available. Mobile vaccination teams may be deployed to fill the gaps. Health organizations, like the Texas Children’s Hospital system use GIS to plan and optimize routes so they can more efficiently serve a larger population.
Both of the current vaccine candidates require two doses for immunity against COVID-19. However, the time between doses is different for each vaccine candidate and the vaccines are not interchangeable. Therefore, it will be essential to understand who has received the first dose of a vaccination, which vaccine they received, and when they are due for the second dose.
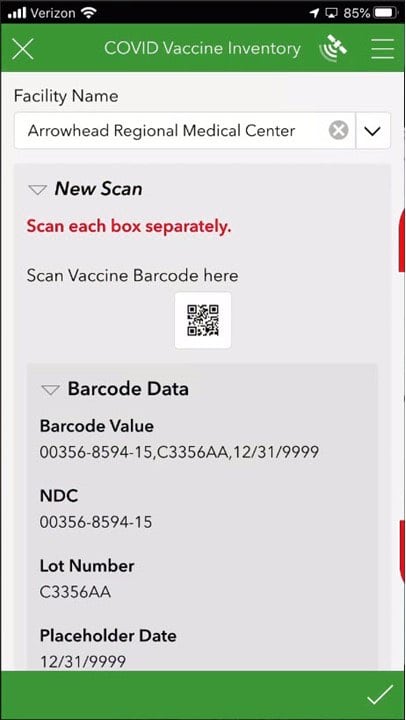
For this, healthcare providers and/or governments will need a quick and accurate data capture system that records individual vaccination information along with the barcode identifying the vaccine carton and/or vial. The data capture system will need to keep pace with the fast-moving vaccination process and support tracking of vaccine supply, expiration dates, and any potential adverse events. In addition to tracking vaccine supply, officials will also need to keep tabs on inventory of personal protective equipment for healthcare personnel and vaccine kits (needles, syringes, alcohol prep pads).
The ArcGIS Survey123 app from Esri offers an easy-to-use option for collecting this data from a smartphone or tablet. Similar to an earlier COVID-19 effort to collect data on hospitalizations and PPE inventories, the app could track vaccines and read 2D barcodes.
All collected data can feed into a web-based dashboard, using ArcGIS Dashboards, to give decision-makers a real-time view of the constantly changing situation.
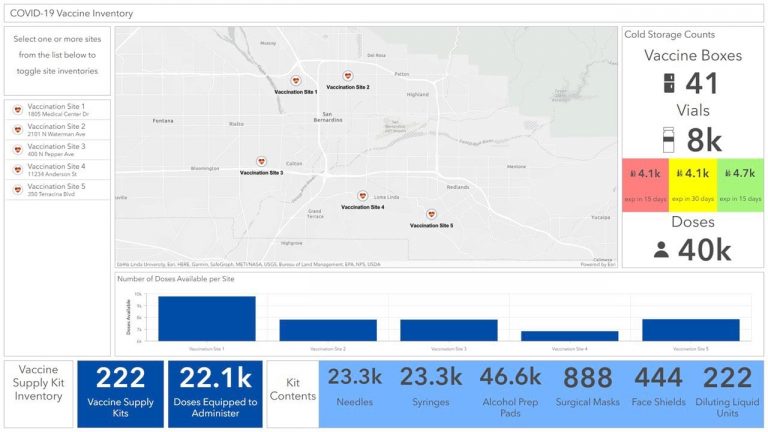
As vaccines are distributed, states and communities will need to know how well each facility is doing in executing the plan, monitoring whether their populations are experiencing adverse events, and tracking the proportion of the community that has been vaccinated.
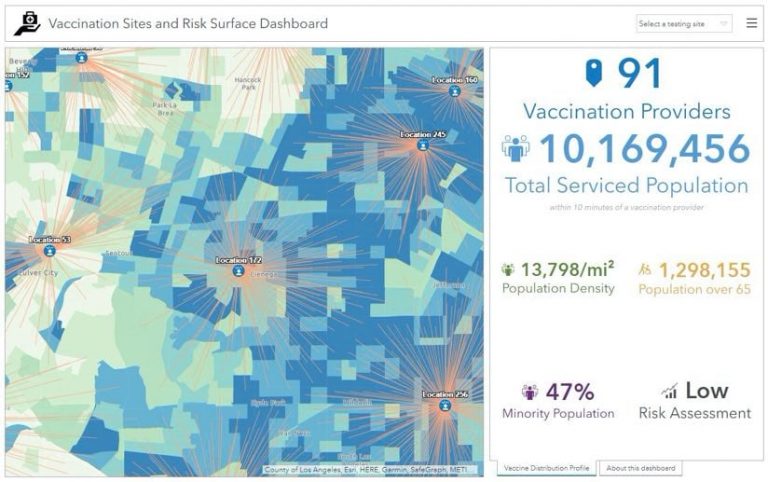
Early transparency will both inspire trust and provide critical information about how and why vaccination resources are allocated in each community. ArcGIS Hub was built specifically as a community engagement platform, offering access to data, maps, and apps related to a designated initiative. For example, the Lake County, Illinois data hub provides an excellent account of crucial COVID-19 information for that region.
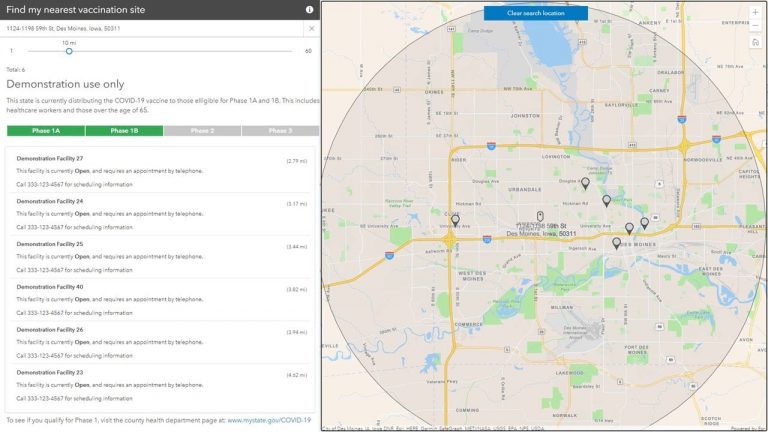
Another feature jurisdictions should strongly consider adding to their ArcGIS Hub site is a vaccination locator service, allowing people to find key information about nearby venues. It could be similar to the map of coronavirus testing sites in this example from the State of California.
Beyond communication to the general public, government leaders will also need to consider targeted outreach to special populations—those with vaccine hesitancy or non-traditional preferences for receiving information. Tapestry Segmentation data from Esri, which goes beyond demographics to offer unique insights into US neighborhoods, can help officials learn more about the needs and communication preferences of their population. By adding Tapestry data to maps, charts, and reports, officials can learn how to deliver relevant and effective messages to their communities.
Governments and responding organizations around the world must consider the aforementioned factors as they develop plans for distributing the vaccine. Communication has to be handled with clarity and great transparency to drive an effective vaccination campaign and strengthen public confidence in the vaccine distribution process.
In a recent memorandum, the National Governors Association encouraged state leaders to take action. “The challenge of vaccine development is matched by the challenge of vaccine distribution… Although a vaccine is not yet available, lessons learned from the acquisition and distribution of COVID-19 diagnostics and therapeutics suggest that governors may want to begin addressing the challenges of mass distribution before its arrival.”
This sentiment is shared and felt around the world, in both government and healthcare. By relying on a GIS technology platform, leaders will be able to prepare for, implement, and manage COVID-19 vaccine distribution to avoid many of the struggles with capacity and communication encountered at the outset of the pandemic.
Try out three new COVID-19 Vaccine Distribution Tools to evaluate population phases, select distribution sites, and select new sites.

June 25, 2020 |

April 7, 2020 | Multiple Authors |

June 2, 2020 |